From consultations to referrals and funding, patient-side AI could change the structure of Australian healthcare faster than the system is ready for.
Clinicians and providers need to upskill in AI and healthcare or risk being left behind, according to panellists at Health Services Daily’s webinar Patient-Side AI Agents: Incremental Tool or System-Level Disruption?
Panellists Bettina McMahon, CEO of Healthdirect, Dr Emily Kirkpatrick, GP and managing director of Ekology Health, Dan Stinton, CEO of Healthengine, and Benedict Kenneally, Asia Pacific lead for Boston Consulting Group, debated whether patient-side AI agents were a marginal support tool, a structural opportunity, or a threat to how Australian healthcare is organised.
Dr Kirkpatrick said the shift was already visible in consultations. She already tells industry colleagues that they need to upskill because “patients are going to be coming in equipped with information, and you just won’t understand and know how to deal with it.”
She said the change was happening so quickly that even the training environment was struggling to keep up.
“I’m supervising particular doctors growing their skillset, helping to grow the GP workforce. I also supervise medical administrators as well.
“The whole way that we learn and the way that we understand healthcare and medicine has just shifted dramatically in the last five months,” she explained.
The panel agreed that the change represented a broader cultural shift, with more patients using AI tools to understand symptoms, treatments, and care pathways before they see a clinician.
“The challenge for that is where does the future of general practice sit and where do we sit as clinicians when we’ve got well educated consumers coming in already knowing or thinking they know what the pathway of their care will be, so it’s going to be a big change ahead of us,” Dr Kirkpatrick said.
Also in today’s edition:
- The geopolitics of pharmaceutical supply chains
- Let nurse practitioners lead UCCs, says nursing college
- National Parkinson’s plan is out – but where is the money to put it into action?
- TGA opens consultation on sunscreen regulation changes
- Medication software vendors get the eNRMC tick of approval
- Melbourne ranked Australia’s best university and medical school
- New way to raise the alarm if a loved one is deteriorating in hospital
- Fresh inquiry to probe NDIS integrity
The information problem
As patients increasingly rely on large language models for health advice, the question is not whether they will use AI, but where the information those tools rely on comes from.
“These models are trained on publicly available information. And there was a website which showed where LLMs draw their answers from the most. The top one is Reddit. The next one is Wikipedia, and the next one is YouTube, because that’s the data available for the training,” Ms McMahon said.
At Healthdirect, they’re having direct conversations with some of these agents so Australians can find relevant information that reflects our clinical guidelines.
“We think [there’s] a way that those engines can reach into our content and other government datasets in a way that is safe, that’s processed onshore, that protects privacy,” she said.
When questioned about AI agents recommending providers directly, 71% of webinar participants agreed it could have many impacts including improving transparency, threatening existing referral pathways, increasing competition and risking safety.
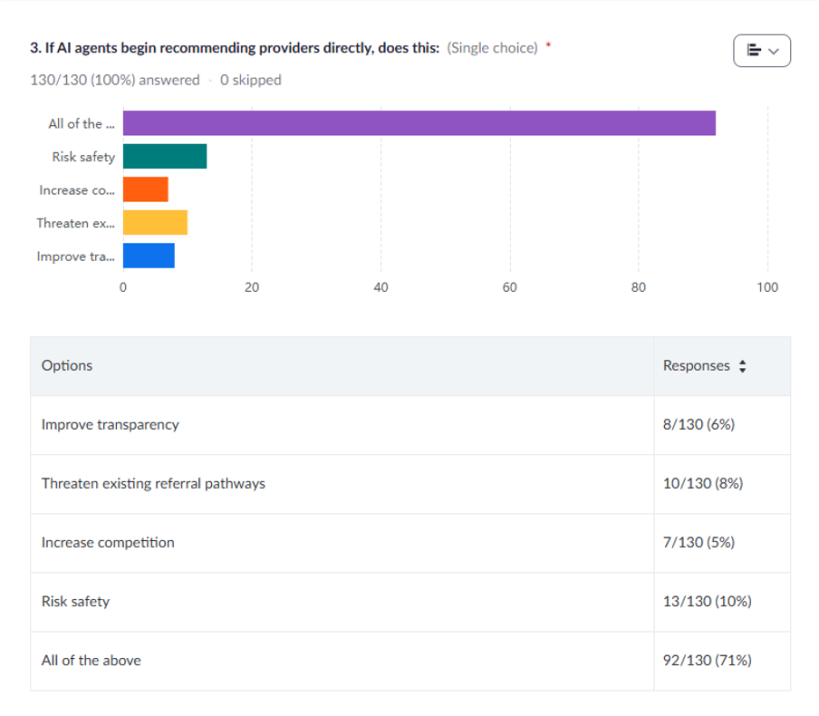
The digital front door is already shifting
The impact is not limited to information. Patient-side AI is beginning to change how people find and access care.
Mr Stinton said Healthengine had already built tools allowing AI systems to connect directly to provider booking systems.
“We’ve built what’s called an MCP server … What that does is it enables tools like ChatGPT and Claude to be able to find a healthcare provider within that environment and then make a booking directly from within that environment,” he said.
Although only 5% of their bookings are coming from LLMs, he expected it to grow.
“That’s still very small numbers in the grand scheme of things, but that’s a pretty big change given how stable Google’s hold on the digital front door has been for a long period of time,” he said.
However, he was circumspect about how quickly the AI growth might be.
“I’m not sure we’re going to be comfortable with a complete AI doctor prescribing medication or some form of robotics, which can carry out the physical examination side of things. I just don’t think it’s going to change as fast as people think,” he said.
The real disruption may come from funding
Mr Kenneally said the extent of change would depend less on technology and more on how healthcare was funded.
“Healthcare systems are basically organised around how people get paid. In Australia that’s largely Medicare. The extent to which this gets disrupted depends on whether you can get paid for doing a task as an AI agent,” he said.
He said AI could make some parts of healthcare easier to access while making others more competitive.
“If all you’re doing is advice, consuming guidelines and learning and research and so on, and bringing it together, the machine can do that.
“If you’ve got unique control over an experience or privately held information, then customers can probably find you more easily, so it offers a growth pathway.
“Alternatively, if you do something that’s still needs a human to do it, but there’s nothing particularly special about it, then it can potentially strip away any premium you have and commoditise,” he suggested.
Related
The more informed patient
Looking ahead, panellists predicted patients would increasingly share their own health data with AI systems in exchange for better advice and personalised care.
“Many consumers will opt to share their personal health record to get better advice … many providers will automate treatment planning and use reminder systems and coaching tools,” Mr Kenneally said.
“But those tools may be commercially available rather than publicly funded, and that creates a risk of a two-tier system emerging.”
This was reflected in the webinar poll results. When asked who should control the primary digital relationship with patients, 62% agreed that patients themselves should.
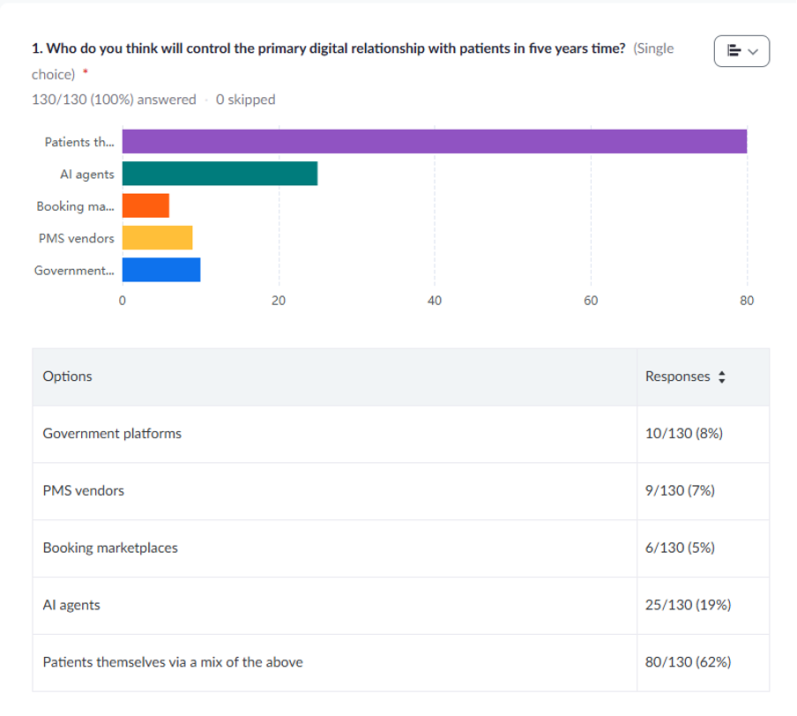
This is where government should come in, Ms McMahon advised.
“At the moment the only option a consumer has is to access the data themselves and put it in, and that’s not acceptable,” she said.
“We need to think about how those engines can reach into trusted data sets in a way that is safe, processed onshore, and protects privacy.”
The panellists believed the shift for patients would be positive, as long as it led to better informed decisions.
“In the end, even when you see a doctor, you’re making a choice about how to care for yourself. The more we empower people to make those choices based on good evidence, the better,” Mr Kenneally said.




