Welcome to the first edition of Grand Rounds, our weekly round-up of news from hospital networks across the country. Want to be featured? Contact cate@healthservicesdaily.com.au
Northern Health, in Melbourne’s outer north, is ditching its paper and pens and going digital with an electronic medical record so that patients “won’t need to repeat their story”.
The new EMR will be going live throughout the network’s inpatient services, at Bundoora Centre, Broadmeadows Hospital, Craigieburn Centre and Northern Hospital Epping.
“This is a huge milestone for Northern Health, and the result of two years of hard work and preparation,” said Siva Sivarajah the CEO of Northern Health.
“Our staff have invested time, skill and effort to design and implement a system that will enable us to provide more timely and efficient care for our patients and community. Thank you for all your hard work and dedication.”
On its website, Northern Health has requested patience from patients during the transition but promise benefits.
“Once we have your information on the record, when you visit next, staff will ask you to confirm (and) update your details, and review your clinical information on the EMR. [The EMR] allows your treating team of clinicians to access your records at the same time for coordinated care, and work together to make the best decisions for your journey at Northern Health,” the website advised.
A Northern Health spokesperson confirmed that Oracle Cerner is the selected vendor.
Cerner’s EMR is used by several other local hospital networks across Victoria, including Western Health, Eastern Health, Austin Health and The Alfred. Cerner is also the current EMR for Queensland Health.
Cerner has recently been unseated as EMR provider for NSW Health but its multiple instances remain in hospitals until the state government finalises the new contract.
Western Australian hospitals use the Opal solution from Altera Digital Health. Altera also provides another solution, Sunrise EMR, to South Australia with rollout expected to be completed at the end of 2024.
In 2022, the Northern Territory started implementation of their Territory-wide electronic patient record system, Acacia – a digital clinical care software based on InterSystems TrakCare.
Tasmania called for tender for a statewide EMR early this year.
Cerner has previously promoted its “plug and play” level of interoperability with third-party applications.
However, Northern Health has confirmed that, at this stage, its Cerner solution is not integrated with any primary care or GPs. However, patient discharge summaries will be electronically shared with GPs after their stay.
Far West NSW LHD
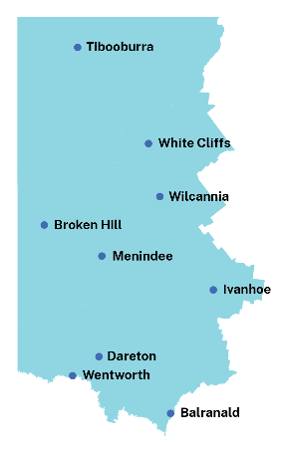
The Far West Local Health District is partnering with Lifeline Connect Broken Hill to deliver a bereavement counselling service to the local community. The new service will provide counselling and individualised support to people experiencing difficulties following the death of a loved one.
Melissa Cumming from Far West LHD, said the bereavement counselling service began on Monday, 4 September.
“The new service is run by Kim O’Donnell who has worked as a counsellor in various roles with non-government agencies over many years,” Ms Cumming said.
“The service is available to people living within the Far West and will use a combination of face-to-face counselling when the counsellor is onsite in Broken Hill, but also via telephone or video conferencing. The service supports people who have experienced the death of a loved one, however, it is not an emergency service.”
Face-to-face counselling will be provided at the Lifeline Connect Centre in Broken Hill (194 Argent Street), on a periodic basis initially. Once established, travel to other areas in the district will be available and bereavement support groups set up.
Self-referral to the service is encouraged, and a referral from a GP is not required. Agencies can refer to the BCS on behalf of someone else but consent from the person is required. Ms O’Donnell can also provide advice and education to organisations and community groups on loss and grief related to death.
Referrals can be made Monday to Friday, 9am to 4.30pm by phoning Lifeline Broken Hill on 08 8087 7525 or in person at the Lifeline Connect Centre at 194 Argent St Broken Hill.
A rise in viral gastroenteritis cases in the Broken Hill community is also making the news in Far West.
Priscilla Stanley, FWLHD’s director of public health, said there had been an increase in the number of people presenting to hospital with gastro symptoms in Broken Hill, particularly in the 0-4 years age group.
Anyone recovering from gastroenteritis should avoid visiting hospitals and aged care facilities to avoid spreading the infection to those most vulnerable. Any person living in a household affected by gastroenteritis should refrain from visiting these high-risk areas until at least 48 hours after the last person in the household has recovered.
For more information visit: www.health.nsw.gov.au/Infectious/gastroenteritis/Pages/default.aspx
Eastern Health
Melbourne hospital network Eastern Health is offering a combined surgery service to help patients with endometriosis to access care.
Gynaecologists and laparoscopic surgeons Dr Shamitha Kathurusinghe and Dr Lior Levy, along with Dr Naseem Mirbagheri and Dr Vinna An from the Eastern Health colorectal team, have initiated the service to offer surgery for patients with severe endometriosis and bowel involvement.
“Patients with endometriosis can have severe disease that causes significant start scarring across many of their organs, and this surgery is highly complex,” said Dr Kathurusinghe.
“In Melbourne there are sites that perform this combined surgery but for the Eastern corridor of Victoria, this has not been the case. Having this service means that patients can actually have surgery close to their home, knowing that we are still providing the expert level care that they deserve.”
The combined endometriosis and bowel surgery service gives hope to people who have been waiting for surgery across both areas of their body impacted by the chronic health condition.
“One of our pertinent practices is to avoid injury such as a bowel injury,” said Dr Kathurusinghe.
“When patients have endometriosis involving the bowel, it can go straight through the bowel, causing significant concerns for the patient but also for us as surgeons. Having the colorectal team support us by doing the surgery together, means that we’re having better patient outcomes, we’re performing safer surgery and the patients actually end up receiving the adequate treatment.”
While endometriosis causes constant and debilitating pain to those suffering from the condition, impacts on the bowel can lead to further complications.
“Having this surgery means they can have the procedure done in a minimally invasive way means that patients can have the disease completely treated, lead to a return back to their quality of life,” said Dr Kathurusinghe.
“When this combined surgery is done, it is curative for some patients; it’s life changing for them.”
Cairns and Hinterland HHS
Cairns Hospital’s emergency department expansion has been completed, with the newest area starting patient treatment from 28 August.
Cairns and Hinterland Hospital and Health Service CEO Leena Singh said the entire $24.5 million project, including upgrades to the existing ED, was on track for delivery early next year.
“Our overall ED upgrade will deliver additional capacity increasing number of available beds from 47 to 53 beds; a dedicated x-ray suite; refurbished resuscitation bays; [an] additional procedure room; and upgrades to waiting areas, storage and staff facilities,” Ms Singh said.
“The new area will provide six treatment areas and a new procedure room with increased isolation and negative pressure capacity.
“While further refurbishment is completed the new area will temporarily provide resuscitation capacity and a separate Queensland Ambulance Service entrance.
“The final stage will include upgrades to the supporting areas, offices, and tearooms for our expanding workforce.”
Ms Singh said the project would expand the capacity of the ED to care for increasing numbers of patients.
“Cairns Hospital is the largest major hospital in far north Queensland, providing emergency care to a region double the size of Tasmania,” she said.
“The hospital’s ED experienced its busiest day in history on 2 May 2022, with a total of 314 patients seeking emergency care; and we have been edging towards that number in recent weeks.
“With a growing population and Cairns an increasingly popular holiday destination, we know this number is only going to keep getting bigger, so we need to grow the ED to keep up.”
The ED upgrade is in addition to the $250 million Cairns Hospital Expansion Project, which includes a refurbishment of wards, a new 32-bed surgical centre, the new 45-bed subacute care facility that opened in Manoora in April, an additional 141 overnight beds and 16 same-day beds/bed alternatives.
Dr Nora McCullagh, Cairns Hospital’s acting director of emergency medicine, said ED staff had been key to the planning process and the complex staged construction program of the expanded facility.
“Since day one, we have tried to do things with as little interruption to our staff and patients as possible, ensuring all areas of the ED have still been able to be used throughout construction, to avoid any reductions in bed and treatment space,” she said.
“That everything is still on track is a testament not only to the professionalism and skill of the builders, but also our staff. We look forward to everything being completed by the early next year.”
Do you have a story tip for us, or a topic you would like to see us cover? Contact the editor at editor@healthservicesdaily.com.au.