Nearly half of all Australians live with at least one chronic condition, and far too many are falling through the cracks.
In March, the Australian Government published the National Strategic Framework for Chronic Conditions, a document that articulates something GPs and patients with chronic conditions could tell you without downloading the polished PDF: Australia’s chronic disease burden is large, growing, and difficult to manage at a system level.
On any given day, GPs may have hundreds of patients on active management plans, alongside patients with chronic conditions and no plan in place. Without infrastructure to actively track these plans, it is difficult to know which patients are overdue, which have a forthcoming appointment that could serve as a review visit, and which have disengaged since their last plan item was billed.
The reviews that do occur are largely initiated by patients. That works well enough for the engaged patient who books ahead and knows what they’re due for, but not for the patient who is struggling to self-manage, or simply unaware their plan review is overdue. Ironically, those are exactly the patients for whom structured, proactive review matters most.
The National Strategic Framework identifies data as a core enabler of better chronic condition management and calls for health systems to be responsive rather than reactive. A system that waits for patients to plan their own chronic disease reviews is not responsive. It is passive, and passivity in chronic condition management has clinical consequences.
The core issue
Ask any practice manager how many patients on their panel are overdue for a Chronic Condition Management Plan (CCMP) review. Most cannot answer that question without running a manual audit, cross-referencing billing records, or spending time they don’t have on a problem that should be solved by infrastructure. And GPs: before you phone your practice manager to demand they step up their game, it’s not their fault. This is a data visibility issue, not a workforce issue.
The Framework outlines that practices should be using clinical data proactively, not retrospectively. Most are not, and it’s not because they don’t care, but rather because the tools to do so have historically not been part of GP software.
The introduction of the GP Chronic Condition Management Plan (GPCCMP) dashboard in MediRecords Clarity addresses this directly. Matthew Galetto, the CEO of MediRecords, noted, “I’ve always cared about helping our customers get more out of the data they already hold. Bringing secure, embedded analytics straight into MediRecords is a big step in that direction.” He further shared, “Having previously founded a clinical data analytics business, this feels like a natural evolution for MediRecords.”
What is the GPCCMP dashboard?
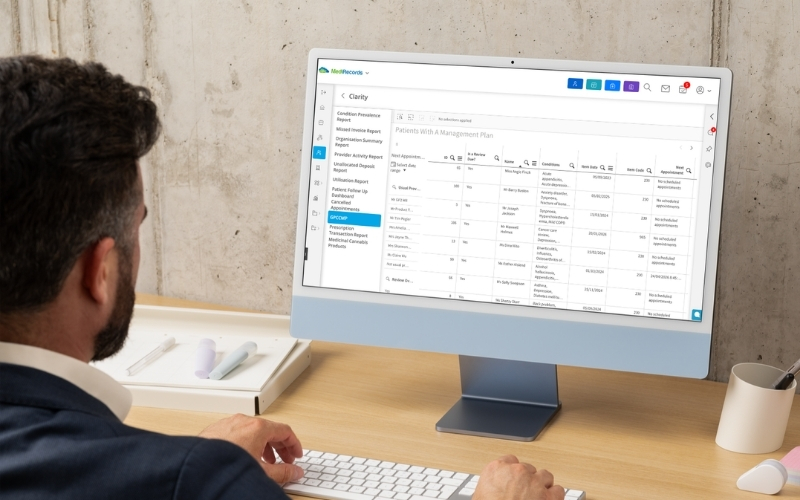
For every patient on an active CCMP, the dashboard shows the plan item, its date, whether a review is currently due, and the patient’s next appointment. It automatically sorts by plan date, with the oldest at the top, so the patients most in need of a review appointment are visible without any manual work.
The dashboard automatically applies the MBS 90-day rule for CCMP reviews, and in under a minute, delivers a clear yes or no on which patients are currently eligible for review.
Highlighting the impact of this innovation, Mr Galetto explained “The real opportunity now is turning visibility into action, helping practices uncover insights that genuinely improve patient outcomes.” This focus on actionable data enhances the overall care for patients with chronic conditions. For a GP, the dashboard makes plan management repeatable rather than an ad hoc audit. For a practice manager, it answers the quality-improvement question that currently has no clear answer: how consistently is this practice proactively reviewing its chronic care patients?
Money makes the world go round (and keeps bulk billing viable)
If CCMP reviews are only happening when patients book them, practices are leaving money on the table. MBS items 965 and 967 attract a scheduled fee of $156.55, whereas item 23 only attracts $43.90. Every overdue review is a consultation that didn’t happen, and every review billed as a regular appointment is a provider underpaid for their time and expertise. For a practice with a substantial chronic disease caseload, this adds up quickly.
The larger, often invisible problem sits one layer deeper. Some patients in your system meet the clinical threshold for a chronic condition (as defined by the Australian Bureau of Statistics) but have never had a GPCCMP initiated at all. They are carrying a documented chronic condition, receiving no structured management support, and generating no plan-related billing. Here, we see both a care gap and a revenue gap occupying exactly the same space.
An upgrade to the GPCCMP dashboard to surface this cohort is currently in testing within MediRecords Clarity and will give practices a direct view of their patient cohort without chronic disease management. For practices that have never audited this group, the number is rarely zero.
Your data should be working for you
The National Strategic Framework sets the direction, and the MBS provides the mechanism. What GPs have lacked is the infrastructure to ensure consistent delivery without adding to their already stretched teams.
MediRecords Clarity provides that infrastructure, using data already inside your database. It is a reporting and analytics layer built directly into MediRecords, designed to surface the clinical and operational data practices already hold, but rarely see in a format that drives action.
The GPCCMP report is just one of several available in Clarity, with more in development. Each applies the same core principle: your data already exists inside your practice management system. It should be working for you.
MBS item fees are indicative. Confirm current scheduled fees at mbsonline.gov.au. The National Strategic Framework for Chronic Conditions (March 2026) is available at health.gov.au.
This article is sponsored by MediRecords.


